-
COVID-19 Advice
-
Resources
-
Frequently Asked Questions
-
Science Behind COVID-19
-
Business Continuity Planning
-
Financial Assistance
-
Compliance Activities
FAQs 2024
-
COVID-19 Advice
Last updated: 5 January 2022
Our COVID-19 web pages and documents were current at the time of publishing. The information provided is routinely reviewed by Safe Food however, given the evolving nature of the pandemic and the government response, some of the information may not reflect the latest COVID-19 government advice.
Australia actively responding to the COVID-19 pandemic. COVID-19 is a respiratory illness spread from person-to-person contact and through direct contact with respiratory droplets from an infected person (e.g. when they cough or sneeze).
There is no evidence to date to suggest that food is a source or route of transmission of the virus. It is also highly unlikely that a person can contract COVID-19 from food or packaging.
Reduce the risk of COVID-19 transmission by maintaining physical or social distancing, limit the time of exposure, maintain good ventilation and practise good hygiene.
Vaccination and agribusinesses
For information on vaccination and protecting agribusinesses against COVID-19, refer to the Department of Agriculture and Fisheries (DAF) vaccination page.
Border restrictions and class exemptions
Agribusinesses should review their plans to cross the border, unless vital, in order to reduce the risk of spreading COVID-19. Please refer to the DAF Queensland border restrictions and class exemptions page.
Review your COVID-19 plans regularly
The science around COVID-19 and its transmission is rapidly evolving. Safe Food recommends that you regularly review your COVID-19 related plans and procedures to ensure they are updated to reflect the most current advice. While the principles that have informed the advice on our website remain correct, some definitions in current use have changed.
For instance, the definition of a close contact has been updated.
The advice to reduce the risk of transmission of COVID 19 continues to be:
- Stay home if you are sick
- If you have any COVID-19 symptoms, no matter how mild, get tested
- Stay 1.5 metres away from other people
- Wash your hands often, using soap and water or hand sanitiser
- Sneeze or cough into your arm or a tissue then put the tissue in the bin and wash your hands
- Wear a face mask when you are not able to keep 1.5 metres away from other people or whenever mandatory face masks are required.
Safe Food advises you to check the QLD Health website and Department of Health website for the most up to date information.
For consumers
Consumers are advised to monitor and follow health advice. If you develop a fever, a cough, sore throat or shortness of breath, contact a doctor or call 13HEALTH (13 43 25 84).
There is no reason to avoid certain foods or specific cuisine as a result of COVID-19.
Good hygiene is important in helping protect yourself against infection and stop the virus from spreading. Wash your hands frequently and thoroughly. Practice social distancing by staying at least 1.5 metres away from others as much as possible.
Please visit the Australian Government’s Department of Health website for more advice. For information specific to Queensland, visit the Queensland Government’s COVID-19 hub.
For food businesses
All food businesses in Queensland are required to meet the requirements of the Food Standards Code. Workers are advised to follow health advice and stay home if you are sick.
Food businesses are encouraged to consider what contingencies can be put in place to reduce workforce impacts caused by COVID-19. The following resources have been developed to assist you:
 Guideline for Responding to a Confirmed Case of COVID-19
Guideline for Responding to a Confirmed Case of COVID-19
 Executive Summary for Guideline for Responding to a Confirmed Case of COVID-19
Executive Summary for Guideline for Responding to a Confirmed Case of COVID-19
 Guideline for Reducing Workforce Impacts Related to COVID-19
Guideline for Reducing Workforce Impacts Related to COVID-19
 COVID-19 Impact Mitigation Program Outline and Risk Matrix
COVID-19 Impact Mitigation Program Outline and Risk Matrix
 Checklist for Reducing Workforce Impact from COVID-19
Checklist for Reducing Workforce Impact from COVID-19
 Communication Advice for a Food Business for a Confirmed Case of COVID-19
Communication Advice for a Food Business for a Confirmed Case of COVID-19

Managing COVID-19 in workplaces (QLD Gov)
What is Safe Food doing?
Safe Food is working with other Queensland agencies to provide a whole of government approach to managing and assisting with the impacts of COVID-19. This has included development of a Response Protocol for a Confirmed Case of COVID-19 at a Red Meat Processing Establishment.
Safe Food is continuing to undertake its regulatory activities in accordance with the latest health advice from Queensland Health. The production of food is considered an essential service by the Queensland Government and maintaining confidence and oversight of food safety in the food supply chain is critical at this time.
Safe Food is also actively engaged in the Queensland Government’s Agricultural Coordination Group, which consists of key food regulatory agencies and industry associations, to ensure an open dialogue between industry and government.
We also continue to provide up-to-date advice here on our website about business continuity planning and financial assistance available from the Queensland and Australian Government.
-
Resources
Our COVID-19 web pages and documents were current at the time of publishing. The information provided is routinely reviewed by Safe Food however, given the evolving nature of the pandemic and the government response, some of the information may not reflect the latest COVID-19 government advice.
Advice for Food Businesses
 Guideline for Responding to a Confirmed Case of COVID-19
Guideline for Responding to a Confirmed Case of COVID-19
 Executive Summary for Guideline for Responding to a Confirmed Case of COVID-19
Executive Summary for Guideline for Responding to a Confirmed Case of COVID-19
 COVID-19 Impact Mitigation Program Outline and Risk Matrix
COVID-19 Impact Mitigation Program Outline and Risk Matrix
 Deep Clean Guide in Response to COVID-19 Exposure (FSANZ)
Deep Clean Guide in Response to COVID-19 Exposure (FSANZ)
Additional Resources
 Poster: How to Hand Wash (WHO)
Poster: How to Hand Wash (WHO)
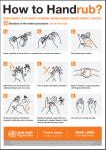 Poster: How to use hand sanitizer (WHO)
Poster: How to use hand sanitizer (WHO)
 Symptoms of COVID-19 (QLD Health)
Symptoms of COVID-19 (QLD Health)
 Poster: How to Stop the Spread of COVID-19 (Australian Dept. of Health)
Poster: How to Stop the Spread of COVID-19 (Australian Dept. of Health)
 Poster: Social Distancing (Australian Dept. of Health)
Poster: Social Distancing (Australian Dept. of Health)
 Checklist: Cleaning Checklist for Businesses (Safe Work Australia)
Checklist: Cleaning Checklist for Businesses (Safe Work Australia)
-
Frequently Asked Questions
Our COVID-19 web pages were current at the time of publishing. The information provided is routinely reviewed by Safe Food however, given the rapidly evolving nature of the pandemic and the government response, some of the information may not reflect the latest COVID-19 government advice.
Safe Food Production Queensland (Safe Food) is working with other Queensland agencies to provide a whole of government approach to managing and assisting with the impacts of novel coronavirus COVID-19. The Queensland government continues to monitor this evolving situation very closely. Your first port of call for accurate, up to date health-related information on COVID-19 is Queensland Health – www.health.qld.gov.au/coronavirus.
-
What is COVID-19?
COVID-19 is a disease caused by a new form of coronavirus known as SARS-CoV-2. Coronaviruses are a large family of viruses that cause respiratory infections. These can range from the common cold to more serious diseases.
-
Should I encourage my employees to get the vaccine?
Vaccination remains the best way to keep our communities and businesses open. Meat processors, seafood and food distribution workers are encouraged to get the COVID-19 vaccine as a high risk worker.
Businesses are encouraged to promote the COVID-19 vaccine to their workers to minimise the risk of business lockdowns, and protect families, colleagues and the community. The vaccine is free for everyone in Australia, even if you are not an Australian citizen or permanent resident.
The COVID-19 vaccine is safe and effective and will protect you from COVID-19. Find out more about the vaccine on the Queensland Government’s vaccination page.
-
Can COVID-19 be passed on from food?
COVID-19 is a respiratory illness spread from person-to person contact and through direct contact with respiratory droplets from an infected person (e.g. when they cough or sneeze).
Current advice from the World Health Organisation (WHO), Department of Health, and Food Standards Australia New Zealand is that COVID-19 is not known to be transmitted by food. It is highly unlikely that a person can contract COVID-19 from food or packaging.
As always good hygiene is the best mechanism to prevent transmission and maintaining effective cleaning of contact surfaces reduces the risk of the spread of the virus.
Further information can be found on the FSANZ website.
-
Can livestock spread COVID-19?
While current information suggests that SARS-CoV-2 originated in animals, there have not been any reports of livestock becoming sick or playing a significant role in the spread of this human disease.
Regular hygienic practices should be followed after being around animals. This includes washing hands after touching animals or working in farm and animal housing environments. If you become sick with COVID-19 you should restrict contact with animals, just like you would with people.
-
Do I need to change any food safety practices in my business?
The best way to prevent the spread of COVID-19 and protect your business is through good hygiene practices and reducing exposure of staff to COVID-19.
Follow your approved food safety program for cleaning and sanitation of your facility and equipment. Thoroughly cleaning all surfaces with water and detergent and applying normally used cleaning agents (e.g. sodium hypochlorite, hydrogen peroxide, and 70% ethanol) is sufficient. No change in concentration or exposure times is needed. Whilst coronavirus is destroyed by hot water (e.g. by dishwashers operating above 60°C [5]), use of hot water for general cleaning and sanitising of surfaces and equipment may pose unnecessary workplace health and safety risks and is therefore not recommended given the above alternatives.
Ensure surfaces such as door handles, handles to refrigerators, taps and other ‘high touch’ areas are subject to frequent and effective cleaning. Consider whether aspects of the Australian Government guidelines for cleaning will add anything to your standard procedures for cleaning and disinfection of the premises.
All staff should be trained in personal hygiene and how to wash their hands properly. A poster is available to display at handwashing stations in your business.
Employees showing signs of infectious illness (such as coughing, sneezing, flu-like symptoms, gastrointestinal illness) must not attend work. It is recommended that the health of all employees be reviewed on a daily basis and any workers showing these symptoms sent home or advised not to come into work.
Refer to Queensland Health’s advice regarding who is most at risk of getting really sick from COVID-19, and practical tips for how people can protect themselves and others.
Consider if there are any higher risk activities in your business that need to be managed and implement appropriate risk management strategies. For example, if you have face-to-face contact with customers, encourage social distancing and have hand sanitiser available for use.
-
How do I prepare my business for the impact of COVID-19 and reduce disruptions to my business operations?
Ensure your staff are exercising good food safety practices and check on their mental wellbeing during this time.
To reduce the impact of COVID-19 on normal business operations, consider the following:
- Ensure your staff know the symptoms of COVID-19 to monitor their own health. A poster is available for download to display in your business.
- Monitor staff absenteeism, staff movements and travel. Stay up-to-date on Queensland’s border restrictions and declared COVID-19 hotspots within Australia. Those who have travelled to hotspots should follow Queensland Government Health advice
- Consider shift sizes, skill ratios and cross training. Where possible, split the workforce or stagger break times to prevent mass gatherings in lunchrooms?
- Can you source alternative suppliers for essential services, ingredients, equipment and PPE? The COVID-19 Supplier Portal can help
- Review staff leave policies and discuss with your staff
- Increase sanitation of common areas such as change rooms, facility entrances and amenities.
The Department of Agriculture and Fisheries (DAF) has established an eHub with business continuity resources to help you prepare for, and respond to, COVID-19 cases at your business. By implementing a business continuity plan you will minimise the impact of the virus on your business.
Also refer to these Guidelines for Reducing Workforce Impacts related to COVID-19.
-
What happens if an employee tests positive for COVID-19 in my business?
Any employee diagnosed with COVID-19 must be isolated and must follow the directions of public health authorities. The employee will be advised by their health care provider as to when they are no longer infectious and can come out of isolation.
It’s likely the employee will have been in contact with other people while infectious. They are deemed infectious two days before symptoms started. If they didn’t have any noticeable symptoms, they are deemed infectious two days before they had the COVID-19 test that was positive. If they have been in contact with co-workers during that period, they need to tell those co-workers they have COVID-19 so they can monitor symptoms and get tested if they feel unwell. Read more about what to do if you have COVID-19
If someone does test positive for COVID-19 in your business, it’s important to respect their privacy where possible and treat their condition with understanding and compassion. Check in on their well-being regularly during self-isolation and monitor their mental health.
In some instances, additional cleaning and sanitising of the workplace may be indicated if an employee returns a positive test. Businesses are advised to follow the Australian Government Department of Health Environmental cleaning and disinfection principles for COVID-19.
For more advice, refer to these Guidelines for Reducing Workforce Impacts related to COVID-19.
-
Science Behind COVID-19
Scientists and authorities across the world continue to investigate COVID-19 and the ways in which it spreads. Safe Food has compiled the following information to assist food businesses and consumers in clarifying sources of risk in the food supply chain.
-
The science behind COVID-19
What is COVID-19?
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is responsible for causing the disease known as COVID-19. This virus was previously known as “novel coronavirus”, meaning it was a new type of coronavirus not previously identified in humans.
Coronaviruses are a large family of viruses. Some can cause respiratory illness in humans, with most infected people experiencing mild symptoms. COVID-19 and other coronavirus types such as MERS (Middle East respiratory syndrome coronavirus) and SARS (severe acute respiratory syndrome coronavirus) can cause more severe symptoms in some people.
How does COVID-19 spread?
There is a lot we still don’t know about COVID-19 and new information about the virus that causes this disease is being discovered every day. The way in which other coronaviruses spread is well known, however.
COVID-19 is a respiratory illness and respiratory droplets from an infected person provide the primary route for transmission of the virus [13].
‘Droplet infection’ via close contact with an infected person is the main way the virus spreads [13][2]. This occurs when the virus is emitted into the air via droplets when an infected person sneezes, coughs, exhales and the virus-carrying respiratory droplets are then inhaled by another person.
‘Smear infection’ is another way that respiratory tract pathogens can spread [2]. This involves people touching their eyes or nose with contaminated hands, leading to infection via the mucous membrane. There are currently no known cases of humans being infected with COVID-19 by other methods [2].
Although COVID-19 genetic material (RNA) has been isolated from stool samples of infected patients, to date there are no reports or any evidence of faecal-oral transmission. Handwashing after using the toilet is always an essential practice especially when working with food [12].
COVID-19 and food
At the present time, there is no evidence or reports of COVID-19 being spread via food. Similarly, there was no evidence of viral transmission through food consumption during previous outbreaks of MERS and SARS [4][5]. There are also no known reports of other coronavirus or respiratory virus infections due to food consumption or contact with food packaging [3][5][13]. Coronaviruses cannot multiply in food [13].
Based on the evidence to date, it is unlikely that transmission of COVID-19 would occur via food. As coronaviruses need an animal or human host to multiply and don’t survive well outside of these hosts, the overall risk of spread from food products is low [2][3]. The likelihood is lower for food products or packaging that are shipped over a period of days or weeks at ambient, refrigerated, or frozen temperatures [2][3].
Whilst it is suspected COVID-19 may have originated in animals, it is not likely to be transmitted to humans from meat in Australia. In Australia all meat sold is subject to strict controls, including requirements that prohibit the use of meat and offal from diseased animals for human consumption. As such, it is unlikely that extra precautions need to be taken for meat in Australia to prevent COVID-19 transmission [14].
Consumers and those that prepare, or handle food are encouraged to continue practicing general everyday hygiene rules to control known food-borne bacteria and viruses. These include:
- washing hands thoroughly and regularly
- covering your mouth and nose when coughing and sneezing
- washing fruit and vegetables prior to eating
- thoroughly cooking meat and eggs
- handle raw animal products with care to avoid potential cross-contamination with other foods
- avoiding close contact with anyone showing symptoms of respiratory illness, such as coughing or fever
Use of soap, disinfectants or detergents to wash food is not recommended. These cleaning products are not designed for human consumption and may be unsafe to use with food.
Those with suspected symptoms of respiratory illness should avoid preparing food for others and seek medical attention.
COVID-19 and animals
Coronaviruses are common in a variety of domestic and wild animals, including bats, dogs, cats, horses, cattle, ferrets and others. Some coronaviruses infect animals only, whilst others can be passed from animals to humans (zoonotic). Occasionally, animal coronaviruses that infect animals have emerged to infect people and then be spread from person to person. This is suspected to have occurred for the virus (SARS-CoV-2) that causes COVID-19. Genetic analyses indicate that SARS-CoV-2 is a close relative of other coronaviruses found circulating in Rhinolophus bat (Horseshoe Bat) populations. However, to date, there is not enough scientific evidence to identify the source of the COVID-19 virus or to explain the original route of transmission to humans (which may have involved an intermediate host) [15].
In the last two major coronavirus outbreaks in humans, transmission was traced to intermediate animal hosts: dromedary camels (MERS) and the masked palm civet (SARS) [7]. Horseshoe bats were found to be the primary reservoir for the virus causing SARS. Emission of coronaviruses into the environment from infected animals via breath or excretions is a possible route of transmission.
Several dogs and cats (domestic cats and a tiger) have tested positive to COVID-19 virus following close contact with infected humans. The World Organisation for Animal Health (OIE) has made these clinical cases available. Currently, there is no evidence to suggest that animals infected by humans are playing a role in the spread of COVID-19 [15].
Studies are underway to better understand the susceptibility of different animal species to the COVID-19 virus and to assess infection dynamics in susceptible animal species, with some studies on cats, dogs, ferrets and fruit bats already completed (see OIE). To date, preliminary findings from studies suggest that poultry and pigs, are not susceptible to SARS-CoV-2 infection [15]. Further studies on larger livestock animals (e.g. cattle) are yet to be conducted.
The current spread of COVID-19 is a result of human-to-human transmission. There have not been any reports of livestock becoming sick with the virus or that they play a significant epidemiological role in this human disease [9]. The predominant route of COVD‑19 transmission appears to be from human to human. Further research is needed to improve understanding of how different animals could be affected by the COVID-19 virus. The World Organisation for Animal Health will continue to provide updates as new information becomes available.
In the interim, if you become sick with COVID-19 you should restrict contact with animals, just like you would around other people. Since animals can spread other diseases to people, standard hygienic practices should be followed being around animals. This includes washing hands after touching animals or working in farm and housing environments.
COVID-19 and surfaces
Specific data on survival of this new type of coronavirus (SARS-CoV-2) on surfaces is limited. Coronaviruses that infect humans have a relatively low environmental stability on dry surfaces. Their persistence in the environment depends on several factors including temperature, surface type, humidity, viral strain, quantity of the virus. Under dry conditions, coronaviruses are generally inactivated within a few hours to several days.
Whilst droplet infection is the main way COVID-19 is thought to spread, it is possible that transmission could occur through smear infections, when a person touches a surface or object that has the virus on it and then touches their mouth, nose or eyes. Based on the above knowledge, smear infection is only likely to occur during a short period after surface contamination.
Very little is known about how the SARS-CoV-2 virus survives outside the human body. Probably the most up-to-date summary of scientific information we have on survival in the environment is from the European Centre for Disease control (ECDC) and the following is a brief summary based on an extract from their recent technical report [16]:
Recent publications have evaluated the survival of SARS-CoV-2 on different surfaces. According to van Doremalen et al., the environmental stability of SARS-CoV-2 is up to three hours in the air post-aerosolisation, up to four hours on copper, up to 24 hours on cardboard and up to two to three days on plastic and stainless steel, albeit with significantly decreased titres. These findings resulted from experiments in a controlled environment and should be interpreted with caution in the real-life environment. Studies show that viral particles are detectable on hospital surfaces in dedicated COVID wards, where the viral load was likely to be high on patient interface surfaces. The virus was detected most commonly on gloves and the studies indicating that fomites likely act as a possible route of transmission however the relative importance of fomites versus direct exposure to respiratory droplets is still unclear.
To minimise the likelihood of transmission by smear infection, general hygiene rules such as regular hand washing, and thorough drying of hands should be followed. Food business employees showing signs of infectious illness should not attend work as per their food safety program and Queensland Health guidelines [8]. Businesses should continue to consistently and correctly clean and sanitise food preparation environments in accordance with their food safety program. The World Health Organisation and International Food Safety Authorities Network (INFOSAN) advise that thoroughly cleaning environmental surfaces with water and detergent and applying commonly used sanitisers and disinfectants are effective and sufficient procedures [12].
Alcohol based sanitisers/surface disinfectants should be used for cleaning purposes. In general, alcohol-based disinfectants (ethanol, propan-2-ol, propan-1-ol) have been shown to significantly reduce infectivity of enveloped viruses like COVID-19 virus, in concentrations of 70-80% with one-minute exposure time. Common disinfectants with active ingredients based on quaternary ammonium compounds (QUATS) and chlorine would also have virucidal properties [17].
A recent review published by researchers in Germany stated that other coronavirus types such as MERS and SARS can persist on inanimate surfaces like metal, glass or plastic for up to 9 days [6]. The researchers concluded that these coronavirus types can be efficiently inactivated by surface disinfection procedures with 0.5% hydrogen peroxide or 0.1% sodium hypochlorite within 1 minute.
Staff engaged in environmental cleaning should wear PPE when performing cleaning activities, such as overalls or uniform, single-use plastic apron, gloves and a face mask. Protective clothing (e.g. uniforms, overalls, etc.) should be frequently washed at 60°C or above [17].
As no specific therapies are available for the virus causing COVID-19, early containment and prevention of further spread is the primary management strategy to stop the ongoing outbreak and minimise potential impacts.
The best approach for all food businesses is to continue to reduce exposure of staff to COVID-19 and adhere to industry best practice for safe food production.
References
- Australian Veterinary Association. “Coronavirus – Australian veterinary Association” [online]. The Australian Veterinary Association Ltd. Accessed 13 March 2020: ava.com.au/coronavirus/
- German Federal Institute for Risk Assessment (BfR). “Can the new type of coronavirus be transmitted via food and toys?” [online]. Bundesinstitut für Risikobewertung. Published 24 February 2020. Accessed 13 March 2020: bfr.bund.de/en/can_the_new_type_of_coronavirus_be_transmitted_via_food_and_toys_-244090.html
- Centers for Disease Control and Prevention (CDC). “2019-nCoV Frequently Asked Questions and Answers – CDC” [online]. U.S. Department of Health & Human Services. Published 12 March 2020. Accessed 13 March 2020: cdc.gov/coronavirus/2019-ncov/faq.html
- European Food Safety Authority (EFSA). “Coronavirus: no evidence that food is a source or transmission route.” [online]. European Food Safety Authority. Published 9 March 2020. Accessed 13 March 2020: efsa.europa.eu/en/news/coronavirus-no-evidence-food-source-or-transmission-route
- Food Standards Australia New Zealand (FSANZ). “Novel Coronavirus and Food Safety” [online]. Food Standards Australia New Zealand. Published March 2020. Accessed 13 March 2020: foodstandards.gov.au/consumer/safety/Pages/NOVEL-CORONAVIRUS-AND-FOOD-SAFETY.aspx
- Kampf G., Todt D., Pfaender S. and Steinmann E. 2020. “Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents”. Journal of Hospital Infection 104: 246-251. doi.org/10.1016/j.jhin.2020.01.022
- Lau S. and Chan J. 2015. “Coronaviruses: emerging and re-emerging pathogens in humans and animals”. Virology Journal 12: 209. DOI 10.1186/s12985-015-0432-z
- Queensland Health. “Fact sheet – novel coronavirus (COVID-19)” [online]. Queensland Health. Published 12 March 2020. Accessed 13 March 2020: health.qld.gov.au/clinical-practice/guidelines-procedures/diseases-infection/diseases/coronavirus/public-info-novel-coronavirus/fact-sheet-coronavirus
- The World Organisation for Animal Health (OIE). “Questions and Answers on the 2019 Coronavirus Disease (COVID-19)” [online]. OIE. Published 2020. Accessed 13 March 2020: oie.int/en/scientific-expertise/specific-information-and-recommendations/questions-and-answers-on-2019novel-coronavirus/
- World Health Organisation (WHO). “Coronavirus” [online]. WHO. Published 2020a. Accessed 13 March 2020: who.int/health-topics/coronavirus
- World Health Organisation (WHO). “Q&A on coronaviruses (COVID-19)” [online]. WHO. Published 2020b. Accessed 13 March 2020: who.int/news-room/q-a-detail/q-a-coronaviruses
- World Health Organisation (WHO). “Infection prevention and control during health care when novel coronavirus (nCoV) infection is suspected – Interim guidance” [online]. WHO. Published 25 January 2020c. Accessed 13 March 2020: who.int/publications-detail/infection-prevention-and-control-during-health-care-when-novel-coronavirus-(ncov)-infection-is-suspected-20200125
- World Health Organization (WHO) and Food and Agriculture Organization (FAO) of the United Nations. “COVID-19 and Food Safety: Guidance for Food Businesses – Interim guidance” [online]. WHO/FAO. Published 7 April 2020. Accessed 16 April 2020: who.int/publications-detail/covid-19-and-food-safety-guidance-for-food-businesses
- Food Standards Australia New Zealand (FSANZ). “Novel Coronavirus and Food Safety” [online]. Food Standards Australia New Zealand. Published March 2020b. Accessed 16 April 2020: foodstandards.gov.au/consumer/safety/Pages/NOVEL-CORONAVIRUS-AND-FOOD-SAFETY.aspx
- The World Organisation for Animal Health (OIE). “Questions and Answers on the 2019 Coronavirus Disease (COVID-19)” [online]. OIE. Published 9 April 2020b. Accessed 16 April 2020: oie.int/en/scientific-expertise/specific-information-and-recommendations/questions-and-answers-on-2019novel-coronavirus/
- European Centre for Disease Prevention and Control (ECDC). “Disinfection of environments in healthcare and non-healthcare settings potentially contaminated with SARS-CoV-2” [online]. ECDC. Published 26 March 2020. Accessed 17 April 2020: europa.eu/en/publications-data/disinfection-environments-covid-19
- The International Food Safety Authorities Network (INFOSAN), private communication, 9 April 2020.
-
Are food and packaging a source of infection for the COVID-19 virus (SARS-CoV-2)?
At the present time, there is no evidence or reports of COVID-19 being spread via food. This is despite the innumerable meals eaten across the globe since the beginning of the pandemic. Similarly, there was no evidence of viral transmission through food consumption during previous outbreaks of MERS and SARS [1][2]. There are also no known reports of other coronavirus or respiratory virus infections due to food consumption or contact with food packaging [2][3][4].
Specific data on survival of SARS-CoV-2 on surfaces, including packaging and food, is limited. Coronaviruses that infect humans have a relatively low environmental stability on dry surfaces and their persistence in the environment depends on several factors including temperature, surface type, humidity, viral strain, quantity of the virus. Coronaviruses cannot multiply in food and don’t survive well outside of a host [4].
Whilst droplet and aerosol infection are the main ways COVID-19 is thought to spread, it is possible that transmission could occur through smear infections, but based on the above knowledge, smear infection (e.g. from food or packaging to mucous membrane) is only likely to occur during a short period after surface contamination.
Most reports to date (with the exception of some experimental studies [5]) have identified presence of the virus on food, without giving an indication of viral load or viability. Other recent publications [6][7] have evaluated the survival of SARS-CoV-2 on different surfaces, but these findings resulted from experiments in a controlled environment and should be interpreted with caution in the real-life environment. The presence of SARS-CoV-2 in food may indicate poor food safety practices but does not necessarily translate into an infection risk for consumers. Primary infection with SARS-CoV-2 is via the respiratory route and foodborne transmission has not been demonstrated.
The current global opinion confirms that the risk of contracting COVID-19 from food, packaging and the environment, while not nil, is significantly lower than the risk of contracting COVID-19 from an infected person. This assertion is consistent with that of the International Commission on Microbiological Specifications for Foods (ICMSF), which concluded from risk-based perspective, that it is very unlikely contamination of food with SARS-CoV-2 would result in infection. This likelihood is even lower for food products or packaging that are transported over a period of days or weeks [3][8].
REFERENCES
[1] European Food Safety Authority (EFSA). “Coronavirus: no evidence that food is a source or transmission route.” [online]. European Food Safety Authority. Published 9 March 2020. Accessed 13 March 2020: efsa.europa.eu/en/news/coronavirus-no-evidence-food-source-or-transmission-route
[2] Food Standards Australia New Zealand (FSANZ). “Novel Coronavirus and Food Safety” [online]. Food Standards Australia New Zealand. Published March 2020. Accessed 13 March 2020: foodstandards.gov.au/consumer/safety/Pages/NOVEL-CORONAVIRUS-AND-FOOD-SAFETY.aspx
[3] Centers for Disease Control and Prevention (CDC). “2019-nCoV Frequently Asked Questions and Answers – CDC” [online]. U.S. Department of Health & Human Services. Published 12 March 2020. Accessed 13 March 2020: cdc.gov/coronavirus/2019-ncov/faq.html
[4] World Health Organization (WHO) and Food and Agriculture Organization (FAO) of the United Nations. “COVID-19 and Food Safety: Guidance for Food Businesses – Interim guidance” [online]. WHO/FAO. Published 7 April 2020. Accessed 16 April 2020: who.int/publications-detail/covid-19-and-food-safety-guidance-for-food-businesses
[5] Fisher D. et al. 2020. “Seeding of outbreaks of COVID-19 by contaminated fresh and frozen food”. bioRxiv: posted 18 August 2020. doi.org/10.1101/2020.08.17.255166.
[6] van Doremalen N. et al. 2020. “Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1”. The New England Journal of Medicine 382(16): 1564-1567. DOI: 10.1056/NEJMc2004973
[7] Chin A.W.H et al. 2020. “Stability of SARS-CoV-2 in different environmental conditions”. The Lancet Microbe 1(1): E10. doi.org/10.1016/S2666-5247(20)30003-3.
[8] German Federal Institute for Risk Assessment (BfR). “Can the new type of coronavirus be transmitted via food and toys?” [online]. Bundesinstitut für Risikobewertung. Published 24 February 2020. Accessed 13 March 2020: bfr.bund.de/en/can_the_new_type_of_coronavirus_be_transmitted_via_food_and_toys_-244090.html
-
Is testing of food, food packaging, and surfaces for SARS-CoV-2 useful in a food business?
There is currently no commonly available test for SARS-CoV-2 in food. However, tests are available for the detection of SARS-CoV-2 components (e.g. RNA) on surfaces and packaging. To date, the World Health Organization (WHO), Centers for Disease Control and Prevention (CDC) and the European Food Safety Authority (EFSA) do not recommend this type of environmental testing for infection control or to support hygiene and sanitation approaches. No official sources in Australia currently recommend the use of this sort of targeted assay as a routine approach to the management of SARS-CoV-2 in a food business.
Current SARS-CoV-2 tests detect fragments of the virus, such as RNA, rather than the virus itself. Therefore, they do not provide direct information on the viability of the virus or viral numbers. Consequently, they cannot be used to directly assess the risk of contracting COVID-19 from the tested sample. These factors should be considered when interpreting test results for COVID-19 exposure health risk assessment purposes.
Scientific opinion indicates the risk of contracting COVID-19 from food, food packaging and the environment, while not nil, is significantly lower than the risk of contracting COVID from an infected person via direct contact or respiratory aerosols. The use of environmental SARS-CoV-2 testing without an accompanying COVID-19 exposure risk assessment might be considered an unnecessary burden for food businesses already facing multiple COVID-19 pandemic-associated challenges.
SARS-CoV-2 testing of food or surfaces in a food business should only be considered where end users have a good understanding of how to interpret results, and the corrective actions required to treat the risk, if detected. SARS-CoV-2 environmental tests cannot be used to provide guarantees that a food, package or site is “COVID-19 free”.
Before commencing an environmental monitoring program for SARS-CoV-2, a food business must have a clear understanding of the purpose of testing, how to interpret results, and what actions should be taken following a positive detection of the virus. An environmental screening procedure for SARS-CoV-2 should consider the difference between routine environmental sampling and testing intended to protect product from potential contact with the virus, as opposed to surveillance for the potential presence of SARS-CoV-2 specifically in a food business where the main objective is to provide confidence regarding management to reduce staff and/or customer exposure risk.
Test methods used to detect SARS-CoV-2 must be reliable, robust, reproducible and validated for use on the surface being sampled and tested. Third party accreditation of the testing laboratory (NATA in Australia and IANZ in New Zealand) for SARS-CoV-2 viral RNA (or other viral component) testing in environmental samples is recommended.
Because these tests detect the presence or absence of viral material (typically RNA), a positive result is only an indication that SARS-CoV-2 was likely present on the tested surface at some time. Test results cannot be used to determine infection and food safety risks of the tested surface, but rather as a hygiene indicator with respect to the potential presence of SARS-CoV-2. Positive test results may be used as an indicator for further investigation of potential sources, e.g. the effectiveness of SARS-CoV-2-specific control measures, including clinical, cleaning and sanitization.
Negative test results do not indicate the absence of SARS-CoV-2, rather that it was not detected on a surface. Results may be used as a general indicator of hygiene status and sanitisation procedure efficacy with respect to SARS-CoV-2.
Enhanced monitoring of surfaces using routine indicators of pathogen contamination and sanitary status (e.g. coliform/E. coli, Salmonella, Listeria, ATP, total [heterotrophic] bacterial counts) in conjunction with SARS-CoV-2 testing may assist with the assessment of the overall efficacy of clinical, sanitising, and hygiene practices, including COVID-19-specific control measures.
In a food business, Good Manufacturing Practices (GMP) and Good Hygiene Practices (GHP) used to prevent pathogen contamination of food, and COVID-19-specific control and clinical measures, described in their COVID-Safe Plan, will reduce the risk of SARS-CoV-2 contamination of food. COVID-19-specific control measures refer to but are not limited to: social distancing; avoiding interpersonal physical interactions; using physical barriers, personal protective equipment (PPE) and personal hygiene etiquette, and providing up-to-date, accessible information on COVID-19-specific control and clinical measures to all staff in a language they can understand. Clinical measures include health checks for staff, and when necessary, isolation and/or quarantine of symptomatic or at-risk staff.
-
Business Continuity Planning
Safe Food is continuing to undertake its regulatory activities. However, as a precautionary measure, we have reviewed our Business Continuity Plan to ensure our agency can remain operational should the COVID-19 situation change. We encourage all accredited food businesses to do the same. Now is the time to prepare and consider what contingencies can be put in place to minimise the impact of COVID-19 in your business. For further information, please see the Department of Agriculture and Fisheries’ agriculture continuity web page.
We encourage you to consider the following:
CLEANING & SANITATION
- The best way to prevent the spread of COVID-19 is through good personal hygiene practices. All staff should be adequately trained in personal hygiene and how to wash their hands properly. It is recommended that reminders and refresher training be undertaken. A poster is available to display at handwashing stations in your business.
- Provide hand sanitizer, anti-bacterial wipes and tissues for staff and encourage regular use of these items.
- Continue to maintain good cleaning and sanitation practices throughout your business. Ensure common contact surfaces and shared amenities, such as door handles, fridge handles, taps, elevator buttons, break rooms, toilets, etc. are cleaned thoroughly and regularly.
BUSINESS OPERATIONS
- What will be your response plan if COVID-19 is associated with your business?
- How will production in your business be impacted in the event of a reduced workforce? Do you need to cross-train your staff to be able to perform other duties?
- Will COVID-19 impact the supply of inputs, ingredients, packaging, chemicals or PPE in your business? Can you source these from a local or alternative supplier if needed?
- Do you have a contingency plan in place should a supplier of essential services be impacted by COVID-19 (e.g. your payroll provider, contract cleaners, transport companies, equipment spare parts, etc.)?
If you are an accredited business with Safe Food and encounter any issues with staff or access to essential services to run your business, please contact us as we may be able to determine who can assist you or provide advice.
LABOUR
- What process do you currently have in place when staff may need to self-isolate?
- Are you monitoring absenteeism of staff for flu-like symptoms? Do your staff know the symptoms of COVID-19? Encourage staff with COVID-19 symptoms to self-isolate and contact a medical facility to get tested.
- How will you support staff who test positive for COVID-19 and need to self-quarantine or care for sick family members? A review of your sick leave, carers leave and annual leave policies may be required. You should also consider implementing a return to work policy for staff who may return after an infectious illness. Businesses should request a medical clearance for staff returning to work for any contagious illness.
- If you employ transient workers on short-term visas, have you got a workforce plan in place to address restrictions on inter-state travel and overseas workers?
- Consider organising flu shots for staff to prevent further illness during flu season.
-
Financial Assistance
The Queensland Government and Australian Government have announced a series of loans and grants for businesses that may be impacted by COVID-19. For more information, please contact the relevant government department listed below.
Queensland Government support for business
The Queensland Government has developed an online tool for businesses impacted by the COVID-19 outbreak to check eligibility for financial assistance and other types of relief.
The parameters within the online tool can also be refined to suit the size of your business with options tailored to suit.
Industry specific relief is also provided where applicable.
There are three categories of options available.
Applications are required for:
- advocacy & support assistance
- financial and business planning mentoring
- grants
- fee relief and fee waivers
- asset write-offs and depreciation
- freight assistance
- digital solutions
- boosting apprenticeships
- indigenous businesses support
- temporary work visa holder assistance
- insurance assistance
- COVID-19 cleaning rebates.
Automatically applied options:
- fee/licensing waivers, refunds and rent deferrals
- boosting cash flow, increasing asset write offs and accelerating depreciation deductions
- local/region-based assistance options.
Advice and other business support:
- industry focussed advice and resources
- essential cleaning and hygiene posters, operational business signage, tools and fact sheets
- animal welfare advice
- support for commercial tenants and landlords
- Business financial counselling, National Debt Helpline, financial resilience webinars and Financial Assistance Hub
- Business impact survey
- ATO relief options to assist you meeting your tax obligations
To access the latest information for Queensland based businesses click here.
Australian Government support for business
A range of assistance and support is also available from the Australian Government including COVID-19 information and resources for Australian businesses.
Government financial assistance and support is being offered in the following areas:
- for small business and sole traders
- for employers
- for specific industries
- for indigenous businesses
Additional resources are available including:
- information on vaccinations, business restrictions and how to keep you, your employees and customers safe
- the top 10 Frequently Asked Questions (FAQs) from business owners
- a guide with steps to take to help keep your business operating in times of unexpected circumstances and disasters.
To access the latest information for Australian businesses click here.
-
Compliance Activities
Safe Food is focused on the health, wellbeing and safety of our staff, accreditation holders, their employees and consumers. We are here to support accredited businesses during the COVID-19 pandemic.
Committed to food safety
We wish to assure accredited businesses that we are committed to supporting you to maintain good food safety practices. During this evolving situation, Safe Food will work with you to ensure that our food safety regulatory arrangements continue in ways that minimise risk and disruption.
We have implemented our business continuity plan to ensure our critical food safety functions continue. Some of the changes we have implemented include:
- The majority of staff are now working remotely to facilitate social distancing
- We’ve limited onsite meetings and are conducting online meetings where appropriate
- Staff have been encouraged to get the COVID-19 vaccine including booster shots where required.
We are also regularly monitoring the COVID-19 situation across Australia and are prepared to manage emerging issues across the food supply chain. Together, we can maintain the reputation of Queensland’s food industry and consumers can remain confident in the safety of the food produced in Queensland.
Continuing our critical business operations
Safe Food has the technology and capabilities to work remotely and have planning in place to ensure our critical business operations continue, and the expectations of consumers and needs of our accreditation holders are addressed.
New applications for accreditation will continue to be processed and managed by the Assessment Team in line with the current legislation.
Food safety notifications and foodborne illness outbreaks will continue to be actioned and investigated by Safe Food officers.
We acknowledge that there is a high degree of uncertainty around the future impacts of COVID-19 and this has caused some concerns for accreditation holders. Safe Food auditors have received requests from industry to follow specific directives before entering a place to undertake compliance activities. Safe Food has also received requests to delay or forgo food safety audits. While we appreciate and acknowledge these concerns, please be reminded that Safe Food’s approved auditors are not present at accredited businesses as “visitors.” Under the Food Production (Safety) Act 2000 they are there to fullfil the obligations of verifying compliance.
We want to reassure all our accreditation holders that Safe Food staff are following the health-related advice of Queensland Health regarding COVID-19. We are here to support you and to assure domestic consumers and overseas markets that essential food safety compliance services will continue in Queensland during the COVID-19 response.

